It is 8:15 PM. Your 3-year-old is in your bed for the fifth night in a row. You said tonight would be the night they slept in their own room. Tonight is also not going to be the night they sleep in their own room. You love them. You also have not slept on your side of the bed in three months.
You are not alone, and your toddler is not broken. Getting a toddler to sleep alone is one of the most common parenting hurdles, and it has an actual playbook — one that doesn't require letting your child cry it out, and one that works reliably for most families within a few weeks.
This guide covers when toddlers are developmentally ready, the gradual fade method that works for almost every family, what to do during the inevitable setbacks, and when independent sleep is genuinely not the right goal yet.

Is My Toddler Ready to Sleep Alone?
Before starting any plan, check that the basics line up. Pushing independent sleep on a toddler who is not ready makes the process harder for everyone.
Readiness signals
- Age 2 or older. The American Academy of Pediatrics recommends room-sharing for the first 6–12 months. After 2, the developmental capacity for short separations is in place.
- Stable daytime sleep and routine. Naps, meal times, and wake-ups happen at roughly predictable hours.
- Healthy attachment. Your toddler can tolerate brief separations during the day (a parent leaving the room, going to the kitchen) without panic. If daytime separations cause severe distress, address that first.
- No major life changes in the past 4–6 weeks. New sibling, move, daycare transition, parent travel, illness. Wait for things to stabilize.
- A safe, comfortable room they actually like. Cool, dark, quiet, with a nightlight if needed. If the room itself feels scary or unwelcoming, fix that first.
Reasons to pause and revisit later
- Your toddler is sick or has been recently.
- Your family is in the middle of a stressful transition.
- Your toddler is in a separation-anxiety phase (often peaks at 18 months and again around 2.5–3).
- A new baby is arriving in the next 2 months.
There is nothing wrong with waiting. Many cultures co-sleep into the preschool years and beyond. The decision to move to independent sleep is a family choice, not a developmental milestone. Once you decide to start, though, consistency is what determines how long it takes.
What to Do Before Night One
The work to set up independent sleep happens in daylight. A few things to put in place during the week before:
1. Talk about it positively, during the day
Three or four short, casual conversations during normal play in the days leading up. "This week we're going to start sleeping in your own bed all night. Loo is going to be there. It is going to be cozy." Avoid making it sound like a big deal — kids read tone. Casual confidence works better than ceremony.
2. Set up the room together
Let your toddler help arrange their bed, pick a special blanket or stuffed animal, choose a nightlight. Buy-in matters. Even small ownership decisions ("the bunny goes on this pillow") shift the child from passive recipient to active participant.
3. Lock in the bedtime routine
A predictable bedtime routine is the single strongest predictor of how smoothly independent sleep goes (Mindell & Williamson, 2018, Sleep Medicine Reviews). Bath, pajamas, teeth, story, lights out — same order, same time, every night. If your routine has been loose, tighten it for a full week before starting. For the full framework, see bedtime routine for toddlers.
4. Make sure they're getting enough sleep
An overtired toddler resists everything, including their own bed. Check your child's total hours against the sleep-by-age guidelines. If they are short, move bedtime earlier first — independent sleep is much easier from a rested baseline.
5. Pick the start date
Friday or Saturday night, or a stretch when you don't have early morning work. The first few nights involve more disruption than usual; lining them up with a slower morning helps.
The Gradual Fade Method
This is the method that works for the largest share of families, with the least short-term distress. It takes 1–3 weeks of consistency.
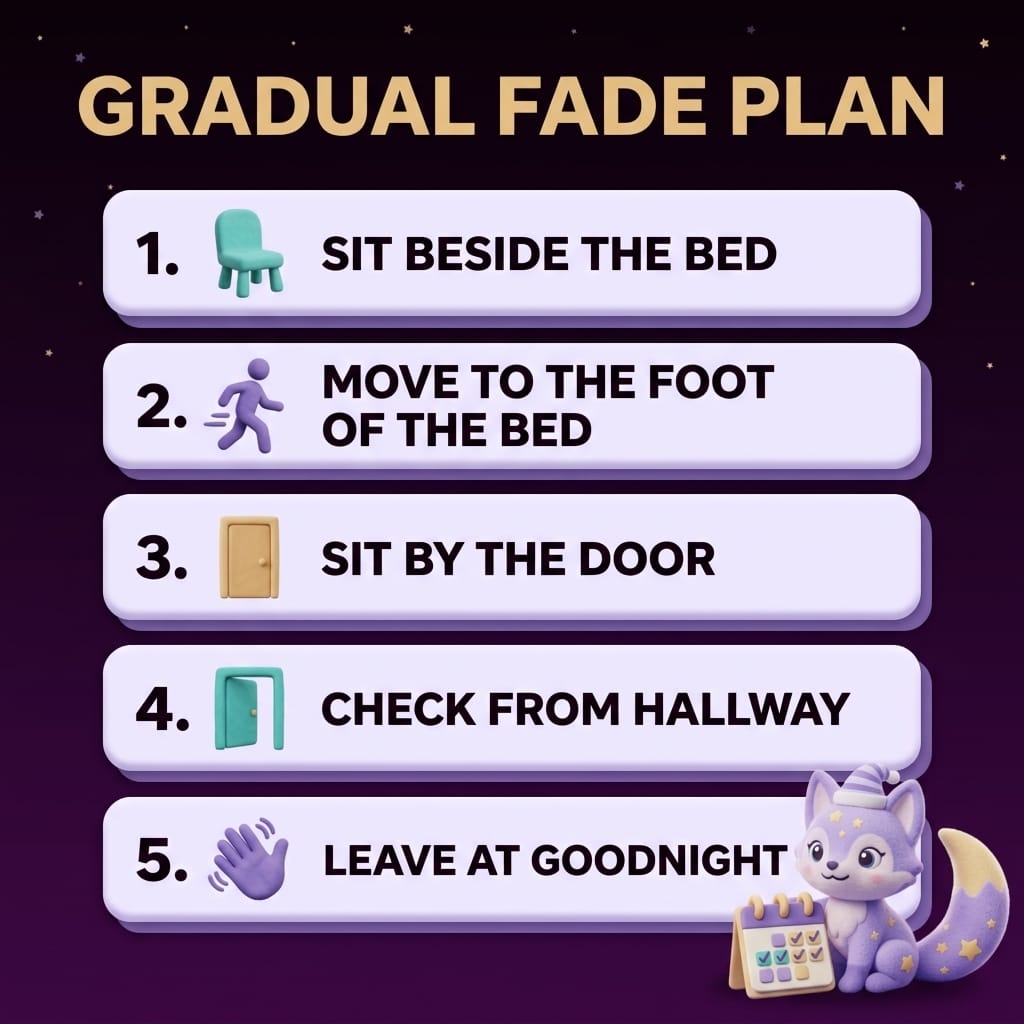
Step 1: Sit beside the bed (nights 1–3)
After your usual bedtime routine, instead of leaving the room or getting into bed with your child, sit on a chair right next to their bed. Read your own book quietly, or close your eyes. Don't engage in conversation. If they speak to you, one short reply: "It is sleep time. I am right here." Stay until they fall asleep.
The goal of this phase: prove to your toddler that bedtime in their own bed is safe. Your physical presence is the proof.
Step 2: Move to the foot of the bed (nights 4–6)
Move your chair to the foot of the bed. Same rules: quiet, undramatic, present. If your toddler protests, the same one-line answer. "It is sleep time. I am right here."
Step 3: Sit by the door (nights 7–9)
Chair moves to the doorway, still inside the room. You're now visible but more distant. Many children mildly protest this transition — that's normal. Hold the boundary kindly.
Step 4: Check from the hallway (nights 10–13)
You leave the room after lights-out, with a single calm "I'm right outside, I'll come check on you." Check in physically every 3–5 minutes at first — quick, calm, undramatic. "You're doing great. Goodnight." Then leave again. Gradually stretch the intervals (5 min, then 10, then 15).
Step 5: Leave at goodnight (nights 14+)
You complete the bedtime routine, kiss goodnight, leave the room, and don't return unless there's a genuine need. By this point your child has the wiring in place to settle on their own. Most families lock in around night 14–21.
The single most important rule
Do not skip steps. Each step is a small, manageable adjustment. Trying to jump from "in bed with my toddler" to "leaving at goodnight" usually triggers a full anxiety spiral. The whole point of the gradual fade is that each step is a small enough change that your toddler's nervous system can adapt to it.
Other Methods (Briefly)
The gradual fade works for most families. Some prefer or need a different approach. Here is the honest landscape:
Check-and-console (Ferber method, modified)
You leave after the bedtime routine. If your toddler cries or protests, you check on them at progressively longer intervals (3 min, 5 min, 10 min, 15 min). The checks are brief and calm. Faster results than the gradual fade for many families (often within a week), but harder on parents emotionally and on toddlers in the short term. Works well with kids who respond to consistency more than presence.
Extinction (full cry-it-out)
You complete the bedtime routine and don't return until morning. Effective in 3–7 nights for many children. Distress is real and significant. Not recommended for toddlers in the middle of a separation-anxiety phase or for kids under 18 months. If you choose this path, do it from a calm, rested place yourself — not as a frustrated "I give up" decision after a hard week.
Co-sleep until ready
Some families wait until the child shows readiness signals (asking for their own bed, sleeping fine elsewhere, expressing pride in independence) and transition at that point. Often happens between ages 3 and 5. Works well in families that don't have a pressing reason to move sooner.
There is no objectively "best" method. The right one is the one you can stick to consistently for several weeks. A gentle method applied consistently beats a faster method applied inconsistently.
What to Do When Your Toddler Won't Stay in Bed
The hardest part of independent sleep is usually not the falling-asleep moment — it is the out-of-bed parade that follows. Drinks. Bathrooms. One more hug. Monsters. They are coming.

The "Silent Return"
When your toddler comes out of bed, the response is the same every single time:
- Minimum talk. One line, calm voice: "It is sleep time. You are safe. I love you."
- Walk them back, don't carry. Walking reinforces the routine. Carrying makes it feel like a trip.
- Tuck them back in. Brief, undramatic.
- Leave again. No conversation.
Repeat. The first night might involve 10–25 returns. The second night, fewer. By the fourth or fifth night, almost none.
The mistakes that prolong this phase
- Negotiating. "If you stay in bed I'll give you a sticker." Sounds like a reward; functions as a negotiation that opens future bargaining.
- Lecturing. "You're a big kid now, you need to..." A tired toddler is not going to absorb logic.
- Showing frustration. Even tone of voice. Toddlers escalate to match your energy.
- Caving on the fifth return. The lesson your child learns is that the fifth return is the magic number. Now you'll get fifth returns every single night. Hold the line — kindly, but firmly.
Pre-empt the common stalls
- Cup of water beside the bed (eliminates "I'm thirsty").
- Bathroom right before tuck-in (eliminates "I have to pee").
- Hug and "I love you" said clearly at goodnight (eliminates "one more hug").
- Nightlight already on (eliminates "it's too dark").
A toddler who has had every stalling tactic preemptively handled has less to negotiate with.
Handling Setbacks
Even after independent sleep is established, expect setbacks every few weeks — especially during:
- Illness or teething. Comfort during illness is fine; just reset the routine within a day or two of recovery. The "illness exception" can quietly become the new normal if you don't actively return to the plan.
- Travel and time changes. Daylight saving, vacations, sleepovers. Expect 2–4 nights of regression after returning home.
- Developmental leaps and growth. Around ages 3, 4, and 5, brain development causes temporary sleep disruptions.
- Big life events. A new sibling, starting preschool, a move, a parent traveling.
The fix is the same each time: return to the plan exactly. No new methods, no exceptions, no co-sleeping "just for tonight" — unless you're prepared to do that every night going forward.
When Independent Sleep Isn't the Right Goal Yet
A few cases where it's worth pausing the plan:
- Active separation-anxiety phase. Some toddlers go through periods where everything is "don't leave." This is developmental and passes. Push during it and you can deepen the anxiety; wait it out and the transition becomes easier.
- Trauma or significant life disruption. A recent loss, divorce, illness in the family. Wait until the family has stabilized.
- Underlying sleep issues. If your toddler is also having frequent nightmares (see how to help a child with nightmares), night terrors (see nightmares vs night terrors), or sleep-disordered breathing, address those first.
- Family preference. Some families want to co-sleep longer. That is a legitimate choice. Independence comes naturally for almost every child eventually.
How Bedtime Stories Help the Transition
The moment between parent leaves the room and child falls asleep is the highest-anxiety part of independent sleep. Silence makes it longer. A familiar, calm voice fills the gap.
A calm audio story playing softly as you leave the room serves three functions:
- It bridges the separation. The voice continues even though you don't.
- It redirects attention. A worried toddler with a story to focus on is less likely to spiral into anxious calling-out.
- It becomes a sleep cue. Over a few weeks, your child's brain associates the story with the act of falling asleep.
Read a book together first, then start a soft audio story as you step out. A pre-recorded calm bedtime audio story is especially useful because it's reliable, screen-free, and has no ads or sudden volume shifts. For more on why audio works specifically for sleep, see audio stories vs reading for kids.
For toddlers with bedtime anxiety, the right kind of story can substantially shorten the transition — see bedtime stories for anxious kids for the specific structure that works.
When to Call the Pediatrician
Most independent-sleep transitions don't need medical input. Reach out if:
- The process isn't progressing after 6–8 weeks of consistent effort.
- Your toddler has nightly intense panic at bedtime, not just protest.
- Underlying sleep concerns — heavy snoring, breathing pauses, frequent night terrors, daytime sleepiness despite enough sleep time in bed.
- Daytime separation anxiety has intensified alongside bedtime resistance.
- Bedwetting that resolved is returning or other regression signals.
- Your instinct says something more is going on.
Pediatric sleep specialists and child therapists can often help with cases that don't resolve through behavioral approaches alone.

Common Questions from Parents
My toddler shares a room with a sibling. How do I do this?
Same plan, slightly adjusted. The gradual fade works even with siblings in the room — the older child usually sleeps through the transition phase, and the protesting toddler still settles in 1–3 weeks. If the sibling is also a young child, talk to them in advance: "We're helping [Name] get used to sleeping in their bed. They might cry a little. You don't need to do anything." Most siblings handle this surprisingly well.
What if my toddler shares our bed and we want to change that?
This is the most common situation. The same gradual fade applies, with one adjustment: start by transitioning to their own bed in your room first (an extra mattress or toddler bed in the corner for a week), then move to their own room with the fade method. Trying to skip both steps simultaneously is too much change at once for most kids.
My toddler has a security item. Should they keep it?
Absolutely yes. Blankets, stuffed animals, soft toys are well-supported as transitional objects (Winnicott's classic concept) and help children manage separation. If they don't have one and would accept one, introduce a small soft animal or blanket a week before starting independent sleep so it's "theirs" before the transition.
Can I lie down next to my toddler in their bed instead of using a chair?
You can, but it generally makes the transition longer. The chair is a slightly more "separate" presence than your body in the same bed; smaller steps from "in the bed" to "out of the room" mean more nights of practice. If you want to start with lying next to them for the first 2–3 nights then move to a chair, that's fine — just don't get stuck at "in the bed" for weeks.
Should I do this with multiple kids at once?
Usually no. Pick one at a time. Independent sleep is a substantial change for both child and parent; running it on two children simultaneously usually means inconsistent application for both and slower results. Start with the older child or the easier child first.